Health Insurance EOB
Veryfi's EOB (Explanation of Benefits) OCR API extracts claims, deductibles, and payment data from any health insurance EOB in seconds. No templates. No manual entry. No humans in the loop.
Get Started for Free Book a Demo
Trusted by the world's leading organizations ↘
EOBs: What They Are and Why They’re Breaking Your RCM.
EOB – Explanation of Benefits
An Explanation of Benefits is the document your health insurer sends after a claim is processed detailing what was billed, what was covered, what was denied, and what the patient owes.
Healthcare organizations process thousands of EOBs every month, yet most still handle them manually by copying deductible amounts, claim IDs, and payment breakdowns into billing systems by hand.
The U.S. healthcare industry spends $83 billion per year on administrative transactions between providers and payers, and there’s a $20 billion savings opportunity waiting for organizations that fully automate manual workflows (CAQH, 2025).
What are the Pain Points?
Nearly 15% of claims submitted to private payers are initially denied and reworking each denied claim costs between $25 and $181 every single time. 41% of providers say at least 1 in 10 of their claims gets denied and most medical group practices have only 40% or less of their revenue cycle operations automated (MGMA, 2024).
Healthcare billing and claims processing contributes to $265 billion in wasted healthcare dollars annually (CNBC / industry estimate). Every misread EOB is a potential underpayment, a billing dispute, or a lost dollar. The pain point is simple: structured data trapped inside unstructured documents, still being processed manually.
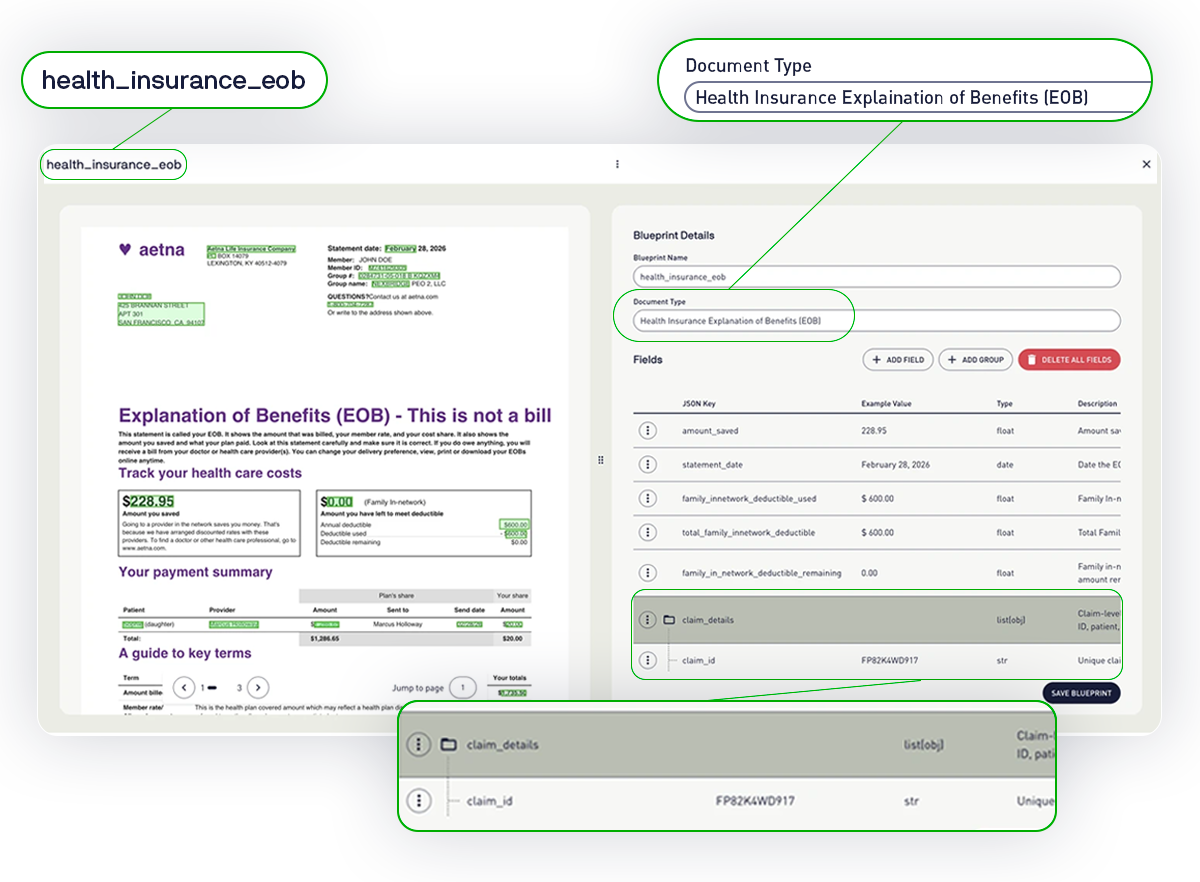
What Data Gets Extracted From Every EOB
Veryfi’s EOB parser returns fully structured JSON for every document, giving you instant access to the data that matters most:
• Statement Date (document issue date)
• Amount Saved (total negotiated savings)
• Family In-Network Deductible Used and the Remaining Amount
• Claim Details (Claim ID, Service date, Provider name, Billed amount, Allowed amount, Provider name and other details)
• Member & Plan Information
EOB Automation Across Every Healthcare Workflow Use Case
Revenue Cycle Management Platforms
The Problem:
• Average cost to rework a denied claim: $25.20
• Denial rates exceed 10% at more than half of U.S. healthcare organizations (MGMA)
With Veryfi:
Automate EOB intake and reconciliation at scale.
EHR & Practice Management Integrations
The Problem:
• Manual processing is on avg 70 min per patient
• $90 billion annual cost of routine administrative (Inovalon and CAQH Index)
With Veryfi:
No manual EOB data posting.
Patient Financial Responsibility Tools
The Problem:
• 60% of patients find medical bills confusing
• Delayed payments and provider switching issues(Becker’s Hospital Review).
With Veryfi:
Surface deductible and cost-share data instantly.
Health Plan Audit Automation
The Problem:
• Medicare FFS recorded $31.70 billion in improper payments in FY2024
• Missing documentation and administrative errors, not fraud (cms.gov)
With Veryfi:
Track claim-level payment accuracy across payers.
Insurance Broker Back-Office
The Problem:
• Claims adjudication costs providers $25.7 billion per year
• $18 billion identified as potentially unnecessary waste (Premier Inc., Dec 2025)
With Veryfi:
Automate remittance reconciliation for group plans.
Healthcare Billing Clearinghouses
The Problem:
• $20 billion in potential savings remains untapped
• 70 minutes processing time per patient (2024 CAQH Index)
With Veryfi:
Process multi-payer EOBs without template maintenance.
Health Insurance Cards OCR API

Automate patient registration and verify coverage eligibility instantly. Extract insurance data to streamline medical billing, reduce claim processing errors, and ensure HIPAA compliance.
Invoices OCR API
Enable 3-way matching with line-item accuracy, transforming your P2P workflows. Supports 91+ currencies, 38+ languages. Extract vendor details, line items, taxes, and payment terms to automate accounts payable processes and improve financial accuracy.
Lab Test Request Form OCR API

Automate test ordering workflows and accelerate laboratory processing. Extract patient demographics, diagnosis codes, and provider details to streamline insurance claims and improve healthcare coordination.
Medical Prescription List OCR API

Automate medication reconciliation and reduce prescription errors. Extract drug names, dosages, and refill information to streamline pharmacy workflows, check drug interactions, and improve patient safety tracking.
Prescription Medication Label OCR API

Enhance medication management and ensure patient safety. Extract dosage instructions, warnings, and expiration dates to enable prescription refills and support adherence programs.
Receipts OCR API
Capture receipts with line item details for 91+ currencies and 38+ languages. Extract merchant information, itemized purchases, taxes, tips, and payment methods to automate expense management and financial tracking.
Trust Matters. Every Patient. Every Document.
-
We don’t just meet global security standards – we exceed them. As veterans in healthcare data processing, we handle your sensitive information with military-grade security while maintaining lightning-fast processing speeds.
Transform your healthcare operations today.
Talk to Veryfi Experts